165 results
Variation of subclinical psychosis across 16 sites in Europe and Brazil: findings from the multi-national EU-GEI study
- Giuseppe D'Andrea, Diego Quattrone, Kathryn Malone, Giada Tripoli, Giulia Trotta, Edoardo Spinazzola, Charlotte Gayer-Anderson, Hannah E Jongsma, Lucia Sideli, Simona A Stilo, Caterina La Cascia, Laura Ferraro, Antonio Lasalvia, Sarah Tosato, Andrea Tortelli, Eva Velthorst, Lieuwe de Haan, Pierre-Michel Llorca, Paulo Rossi Menezes, Jose Luis Santos, Manuel Arrojo, Julio Bobes, Julio Sanjuán, Miguel Bernardo, Celso Arango, James B Kirkbride, Peter B Jones, Bart P Rutten, Jim Van Os, Jean-Paul Selten, Evangelos Vassos, Franck Schürhoff, Andrei Szöke, Baptiste Pignon, Michael O'Donovan, Alexander Richards, Craig Morgan, Marta Di Forti, Ilaria Tarricone, Robin M Murray
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 30 January 2024, pp. 1-14
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Incidence of first-episode psychosis (FEP) varies substantially across geographic regions. Phenotypes of subclinical psychosis (SP), such as psychotic-like experiences (PLEs) and schizotypy, present several similarities with psychosis. We aimed to examine whether SP measures varied across different sites and whether this variation was comparable with FEP incidence within the same areas. We further examined contribution of environmental and genetic factors to SP.
MethodsWe used data from 1497 controls recruited in 16 different sites across 6 countries. Factor scores for several psychopathological dimensions of schizotypy and PLEs were obtained using multidimensional item response theory models. Variation of these scores was assessed using multi-level regression analysis to estimate individual and between-sites variance adjusting for age, sex, education, migrant, employment and relational status, childhood adversity, and cannabis use. In the final model we added local FEP incidence as a second-level variable. Association with genetic liability was examined separately.
ResultsSchizotypy showed a large between-sites variation with up to 15% of variance attributable to site-level characteristics. Adding local FEP incidence to the model considerably reduced the between-sites unexplained schizotypy variance. PLEs did not show as much variation. Overall, SP was associated with younger age, migrant, unmarried, unemployed and less educated individuals, cannabis use, and childhood adversity. Both phenotypes were associated with genetic liability to schizophrenia.
ConclusionsSchizotypy showed substantial between-sites variation, being more represented in areas where FEP incidence is higher. This supports the hypothesis that shared contextual factors shape the between-sites variation of psychosis across the spectrum.
46 Comparison of Anxiety Measures in a Memory Clinic Sample
- Raelynn Mae de la Cruz, Jessica Rodrigues, Rachel M. Butler-Pagnotti, Filippo Cieri, Shehroo B. Pudumjee, Sonakshi Arora, Kimberly L. Cobos, Jessica Z. K. Caldwell, Lucille Carriere, Christina G. Wong
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 725-726
-
- Article
-
- You have access Access
- Export citation
-
Objective:
As the presentation of anxiety may differ between younger and older adults, it is important to select measures that accurately capture anxiety symptoms for the intended population. The 21-item Beck Anxiety Inventory (BAI) is widely used; however, its high reliance on somatic symptoms may result in artificial inflation of anxiety ratings among older adults, particularly those with medical conditions. The 30-item Geriatric Anxiety Scale (GAS) was specifically developed for older adults and has shown strong psychometric properties in community-dwelling and long-term care samples. The reliability and validity of the GAS in a memory clinic setting is unknown. The present study aimed to compare the psychometric properties of the GAS and the BAI in a memory disorder clinic sample.
Participants and Methods:Participants included 35 older adults (age=73.3±5.0 years; edu=15.3±2.8 years; 42% female; 89% non-Hispanic white) referred for a neuropsychological evaluation in a memory disorders clinic. In addition to the GAS and BAI, the Geriatric Depression Scale (GDS) and Montreal Cognitive Assessment (MoCA) were included. Cutoffs for clinically significant anxiety were based on published data for each measure. A dichotomous anxiety rating (yes/no) was created to examine inter-measure agreement; minimal anxiety was classified as “no” and mild, moderate and severe anxiety were classified as “yes.” Internal scale reliability was examined using Cronbach’s alpha. Convergent and discriminant validity were examined using Spearman rank correlation coefficients. Frequency distributions determined the proportion of yes/no anxiety ratings, and a McNemar test compared the proportion of anxiety classifications between the two measures.
Results:Both measures had excellent internal consistency (BAI: a=.88; GAS: a=.94). The BAI and GAS were highly correlated with each other (r=.79, p<.001) and positively correlated with a depression measure (BAI-GDS: r=.51, p=.002; GAS-GDS: r=.53, p=.001). Discriminant validity was supported by lower correlations between the anxiety measures and cognition (BAI-MoCA: r=.38, p=.061; GAS-MoCA: r=.34, p=.098). The BAI classified 14 participants as having anxiety (40%) and 21 participants as not having anxiety (60%), whereas the GAS classified 21 participants as having anxiety (60%) and 14 participants as not having anxiety (40%). The proportion of anxiety classifications were significantly different between the two measures (p =.016). For 28 participants (80%), there was agreement between the anxiety ratings. Seven participants (20%) were classified as having anxiety by the GAS, but not by the BAI; GAS items related to worry about being judged or embarrassed may contribute to discrepancies, as they were frequently endorsed by these participants and are unique to the GAS.
Conclusions:Results support that both anxiety measures have adequate psychometric properties in a clinical sample of older adult patients with memory concerns. It was expected that the BAI would result in higher classification of anxiety due to reliance on somatic symptoms; however, the GAS rated more participants as having anxiety. The GAS may be more sensitive to detecting anxiety in our sample, but formal anxiety diagnoses were not available in the current dataset. Future research should examine the diagnostic accuracy of the GAS in this population. Overall, preliminary results support consideration of the GAS in memory disorder evaluations.
Association between adverse childhood experiences and the number of suicide attempts in lifetime
- J. Andreo-Jover, E. Fernandez-Jimenez, J. Curto-Ramos, N. Angarita-Osorio, N. Roberto, A. De la Torre-Luque, A. Cebria, M. Diaz-Marsa, M. Ruiz-Veguillla, J. B. Bobes Garcia, M. Fe Bravo Ortiz, V. Perez Solá
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S561-S562
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adverse childhood experiences (ACEs), defined as abuse, neglect, or a dysfunctional household in childhood, have been associated with suicidality (Fjeldsted et al., 2020). Every type of ACE has a direct impact on suicide ideation, self-harm and/or suicide attempt (Angelakis et al., 2019).
ObjectivesWe aim to quantify the association between types of ACEs (including emotional, physical, sexual abuse, and emotional and physical neglect) and the number of suicide attempts in lifetime.
MethodsWe included 748 patients who attempted suicide at least once. They were asked to complete the Columbia-Suicide Severity Rating Scale (CSSRS), and the Childhood Trauma Questionnaire-Short Form (CTQ-SF). Logistic regression models were run to assess the association between each ACE type and the number of suicide attempts.
ResultsPoisson univariate regression analyses show a linear trend in the relationship between having a higher number of suicide attempts and having suffered every ACE type in childhood (p<0.05). Our results show a lower percentage of previous suicide attempts among participants without ACEs, and an increasing tendency among patients with various types of ACEs. The rate of ACEs types is significantly higher in the group with previous suicide attempts than in the first-attempt group (p=0.000).
Image:
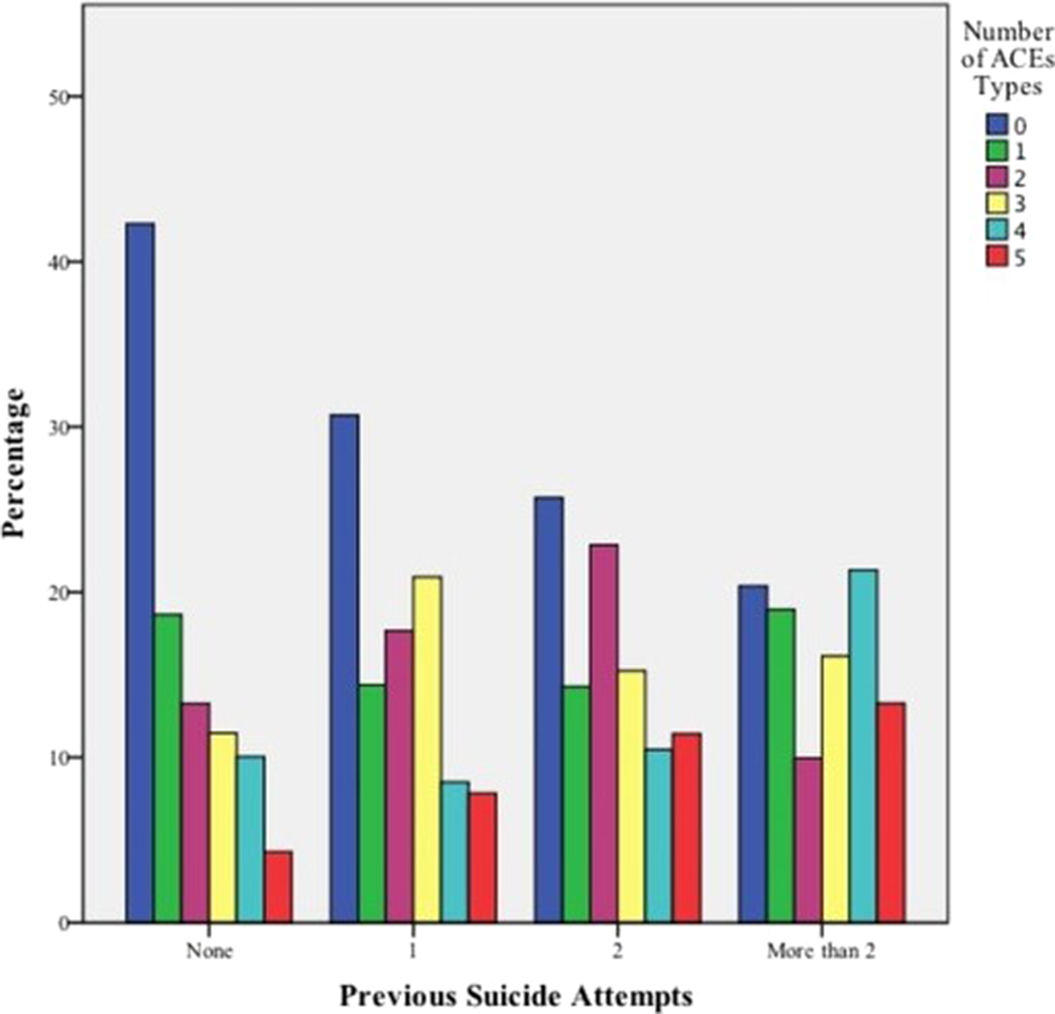
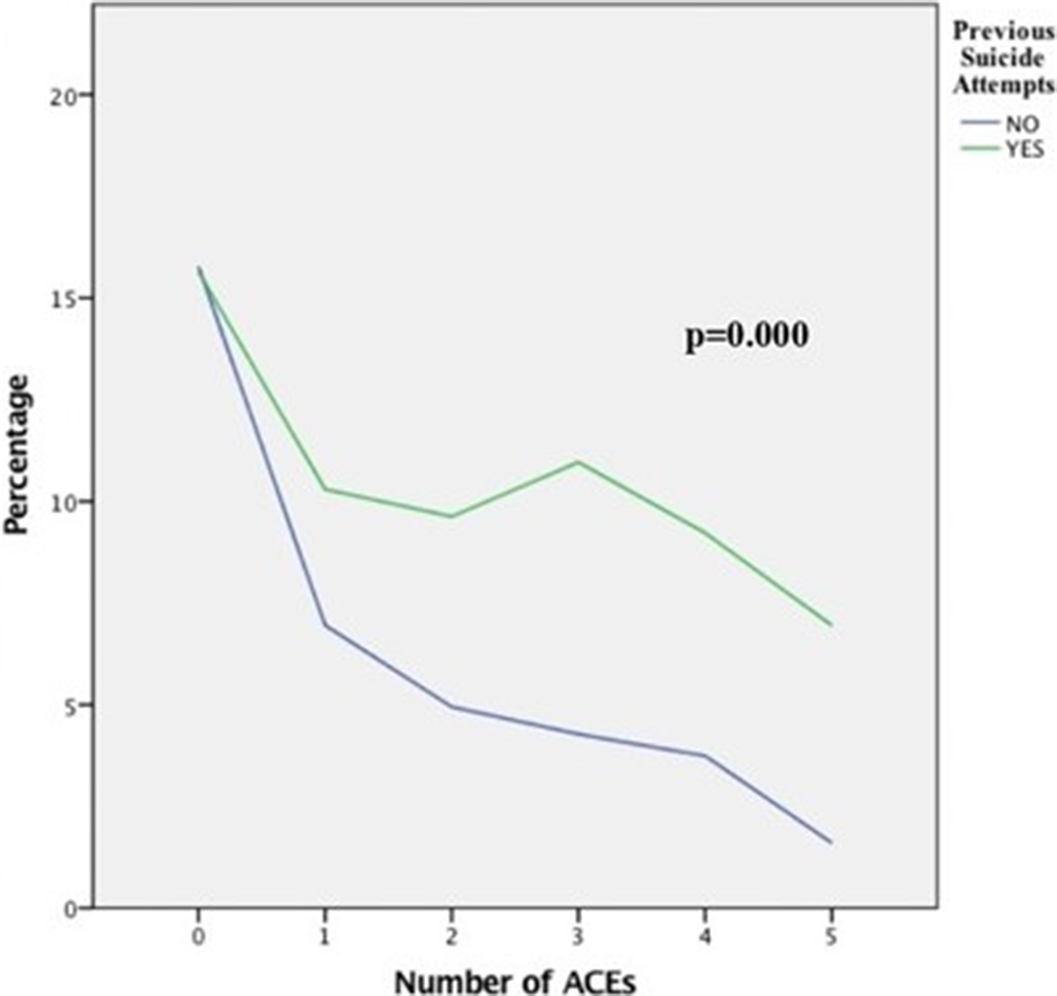
Image 2:
ConclusionsThis study contributes to clarify the role of childhood trauma in the number of suicide attempts in lifetime. This has important implications for reducing suicide rates, and preventing future re-attempts. Further studies analysing every construct of childhood trauma may contribute to the detection of suicidal behaviour.
FundingsThis work was supported by the Instituto de Salud Carlos III (grant number: PI19/00941 SURVIVE) and co-funded by the European Union (grant numbers: COV20/00988, PI17/00768), the European Union’s Horizon 2020 research and innovation programme Societal Challenges (grant number: 101016127), and the Fundación Española de Psiquiatría y Salud Mental
AcknowledgementsSURVIVE project (PI19/00941)
KeywordsSuicide attempt, Adverse Childhood Experiences
ReferencesAngelakis, I., Gillespie, E. L., & Panagioti, M. (2019). Childhood maltreatment and adult suicidality: A comprehensive systematic review with meta-analysis. Psychological Medicine, 49(7), 1057-1078. https://doi.org/10.1017/S0033291718003823
Fjeldsted, R., Teasdale, T. W., & Bach, B. (2020). Childhood trauma, stressful life events, and suicidality in Danish psychiatric outpatients. Nordic Journal of Psychiatry, 74(4), 280-286. https://doi.org/10.1080/08039488.2019.1702096
Disclosure of InterestNone Declared
First-admissions in Psychiatry: a cluster analysis of a sample of inpatients from 2019 to 2021
- E. La Spina, M. Mastrangelo, B. Montalbani, I. Mancinelli, A. Del Casale, A. Comparelli, M. Pompili
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S898
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Only a few studies analyse the clinical and psychopathological characteristics of first-admitted inpatients regardless of diagnosis.
ObjectivesDescribing the psychopathological, demographic, and clinical characteristics of inpatients with acute symptomatology identifying groups with common features using factors extracted from the Brief Psychiatric Rating Scale (BPRS).
MethodsWe selected 103 (48 F) inpatients from the psychiatric ward of the Sant’Andrea Hospital in Rome from January 2019 to December 2021. We assessed psychopathological characteristics and suicide risk with BPRS, Global Assessment of Functioning, and Columbia-Suicide Severity Rating Scale and gathered the anamnestic and demographic data. We conducted descriptive analyses and factor analysis on BPRS items. Then we used the BPRS factors as variables to perform a cluster analysis.
ResultsMajor Depressive Disorder (MDD) was the most frequent diagnosis. We obtained five factors: “Psychotic dimensions” (FI); “Anxiety” (FII); “Hostility and lack of cooperation” (FIII); “Depression” (FIV); “Flattening of affectivity” (FV). We identified two clusters (cluster 1 n=31; cluster 2 n=72). Patients in cluster 1 reported higher average scores in FI and FIII while the average scores of cluster 2 patients in FII and FIV were higher than patients in cluster 1. We called cluster 1 “psychotic and hostile patients compulsory admitted with a low risk of suicide”. Cluster 2 patients are “affective patients with a high risk of suicide”. The two clusters share an average age of 38-39 yo and an average GAF score indicating severe impairment and inability to function in almost all areas. They differ in the psychiatric diagnosis represented: respectively, Schizophrenia Spectrum Disorder and Bipolar Disorder with low suicidal risk, MDD, and Personality Disorders with a high suicidal risk. 39% of patients in cluster 1 were involuntarily admitted.
ConclusionsThe results of our study show that patients admitted for the first time usually are admitted for psychotic symptoms and a high risk of suicide. Psychotic patients more often show hostility and lack of cooperativeness which can explain the higher rate of involuntary admissions. Patients with predominant affective symptoms show a higher risk of suicide. Our analyses do not consider categorical diagnosis highlighting that exist transdiagnostic groups of patients with specific needs.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
Bipolar disorder and substance use: Risk factors and prognosis
- M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga, C. Vallecillo Adame, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. P. Pando Fernández, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder comorbidity rates are the highest among the major mental disorders. In addition to other intoxicants, alcohol is the most abused substance because it is socially accepted and can be legally bought and consumed. Estimates are between 40-70% with male predominance, which further influences the severity with a more complicated course of both disorders.
ObjectivesThe objective of this article is to highlight the impact of substance use on the course and prognosis of bipolar disorder, as well as to make a differential diagnosis of a manic episode in this context.
MethodsBibliographic review of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 45-year-old male patient. Single with no children. Unemployed. History of drug use since he was young: alcohol, cannabis and amphetamines. Diagnosed with bipolar disorder in 2012 after a manic episode that required hospital admission. During his evolution he presented two depressive episodes that required psychopharmacological treatment and follow-up by his psychiatrist of reference. Since then, he has been consuming alcohol and amphetamines occasionally, with a gradual increase until it became daily in the last month. He went to the emergency department for psychomotor agitation after being found in the street. He reported feeling threatened by a racial group presenting accelerated speech, insomnia and increased activity.
ConclusionsThe presence of substance abuse complicates the clinical presentation, treatment and development of bipolar disorder. It is associated with a worse prognosis with multiple negative consequences including worsening symptom severity, increased risk of suicide and hospitalization, increased medical morbidity and complication of social problems. In addition, this comorbidity delays both the diagnosis and treatment, by masking the symptoms, and making more difficult an adequate differential diagnosis.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Long-term neurotoxicity in paediatric patients exposed to general anesthesia: Is there a relationship between exposure to general anesthesia in children between 0 and 4 years of age and the subsequent development of ADHD in childhood?
- B. Hernández Gajate, T. Gutiérrez Higueras, R. M. Fiestas Velasco, V. Rubio de la Rubia, F. Calera Cortés
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S145
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Food and Drug Administration (FDA) recently issued new warnings about the possible effects of the repeated or prolonged use of general anaesthesia and sedatives on the brain development of children under 4 years old during surgeries or paediatric procedures.
ObjectivesTo evaluate the possible long-term neurotoxic impact the exposure to general anaesthesia has on the paediatric population from 0 to 4 years, which is the period during which the brain develops.
MethodsInitially, a search for observational studies that described the risk of neurotoxicity and alterations in the long-term cognitive development of children exposed to general anaesthesia before 4 years of age, was performed in PubMed between 2016 and 2020.
ResultsFinally, 5 retrospective cohort studies comparing children exposed and not exposed to general anaesthesia were included in this study. None of these showed significant differences in their main study variables. However, three of this studies found significant differences in some of the secondary variables such as speed of processing, motor skills, internalization of behaviour and learning, and attention deficit hyperactivity disorder (ADHD).
ConclusionsIn vitro and in vivo studies of anesthetics have shown serious neurotoxic effects in the developing brain. However, the clinical relevance of these findings for children undergoing anesthesia remains unclear.
Most of these studies suggest a strong relationship between exposure to anesthesia in children aged 0 to 4 years, this being greater after multiple exposures. Despite these results, many of these articles conclude that further research is needed on this topic.
Disclosure of InterestNone Declared
PEAKS AND VALLEYS: BIPOLAR DISORDER, RAPID CYCLERS AND ENERGY DRINKS CONSUMPTION
- M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martinez Gimeno, P. Pando Fernández, B. Rodriguez Rodriguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. D. C. Vallecillo Adame, T. Jimenez Aparicio, C. de Andres Lobo, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S702-S703
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar Disorder (BD) is considered a serious mental disorder characterized by a changing mood that fluctuates between two completely opposite poles. It causes pathological and recurrent mood swings, alternating periods of exaltation and grandiosity with periods of depression. We talk about rapid cyclers when four or more manic, hypomanic or depressive episodes have occurred within a twelve-month period. Mood swings can appear rapidly. Approximately half of the people with bipolar disorder may develop rapid cycling at some point.
ObjectivesPresentation of a clinical case about a patient with Bipolar Disorder with rapid cycling and poor response to treatment.
MethodsReview of the scientific literature based on a clinical case.
Results33-year-old male, single, living with his mother, under follow-up by mental health team since 2012. First debut of manic episode in 2010. The patient has filed multiple decompensations related to consumption of toxics (alcohol and cannabis). Currently unemployed. He attended to the emergency service in June 2022 accompanied by his mother, who reported that he was restless. The patient refers that he has interrupted the treatment during the vacations, having sleep rhythm disorder with abuse of caffeine drinks. Currently the patient does not recognize any consumption.The patient reports that during the village festivals he felt very energetic, occasionally consuming drinks rich in taurine and sugars, even having conflicts with people of the village. Finally, the patient was stabilized with Lithium 400 mg and Olanzapine. In September, the patient returned to the emergency service on the recommendation of his referral psychiatrist due to therapeutic failure. The only relevant finding we observed in the analytical determinations were low lithium levels (0.4 mEq/L). The transgression of sleep rhythms and the abuse of psychoactive substances required the admission of the patient to optimize the treatment (Clozapine, Lithium, Valproic Acid). At discharge, he is euthymic, has not presented behavioral alterations and is resting well. Finally, it was decided that the patient should go to the Convalescent Center to continue treatment and achieve psychopathological stability.
ConclusionsBipolar disorder is an important mental illness, having an incidence of 1.2%, being responsible for 20% of all mood disorders. Therefore, it is important to perform an adequate and individualized follow-up of each patient. Treatment with mood stabilizers tries to improve and prevent manic and depressive episodes, improving chronicity and trying to make the long-term evolution as good as possible, being important psychoeducation and psychotherapy.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
Memory complaints and quality of life in a patient with mild cognitive impairment
- M. P. Pando Fernández, M. A. Andro Vidal, M. Calvo Valcarcel, P. Martinez Gimeno, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, C. De Andrés Lobo, T. Jimenez Aparicio, C. Vilella Martin, M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S937-S938
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Subjective memory complaints remain a relevant aspect to be considered in patients with mild cognitive impairment. Likewise, their association with depressive symptoms, quality of life and cognitive performance is also an objective to be studied in such patients.
ObjectivesOur clinical case represents just one opportunity to study how memory complaints are related to depressive states and how they affect the quality of life of patients with mild cognitive impairment.
MethodsWe conducted a bibliographical review by searching for articles in Pubmed.
ResultsPERSONAL HISTORY: Male, 73 years old, separated, residing alone in Valladolid. He has home help, a person comes to help him with the household chores. Little social and family circle.
History in Mental HealthHe has a history of an admission in 2013 to this Short Hospitalization Unit for ethanol detoxification. Since then, he has been followed up in the Mental Health Unit. According to the reports, he has been diagnosed with depressive disorder and cluster B personality disorder.
Current psychopharmacological treatment: diazepam, olanzapine, duloxetine 60 mg, quetiapine.
Toxic habits: history of chronic ethanol consumption. Smoker. He denies other toxic habits.
Current EpisodeThe patient presents a worsening of his mood of 15 days of evolution, coinciding with a voluntary decrease of his psychopharmacological treatment that the patient has carried out on his own. He walks with the aid of a crutch. Hypomimic facies. Slowed language, circumstantial, with speech focused on current discomfort.
On assessment, he reports initial improvement after reducing his medication, but in recent days he has experienced a decrease in initiative accompanied by feelings of emptiness, sadness and loneliness. He refers to memory complaints for which he is awaiting evaluation by Neurology. The patient explains that at other times in his life he has presented self-harming ideas that he has been controlling. At this time he expresses desire for improvement and adequate future plans, and accepts plans to attend a memory workshop. He also reports visual hallucinations with no affective repercussions and preserved judgment of reality.
Therapeutic PlanTreatment adjustment: Duloxetine 60 mg, 2cp/day. The patient is recommended to lead an active lifestyle and attend a day center or memory workshop.
ConclusionsIn numerous patients with mild cognitive impairment, we have observed that memory complaints are closely related to depressive symptoms and to the patient’s functioning in daily life.
In one study memory complaints were a negative predictor of quality of life in these patients.
Therefore, in addition to considering the importance of treating depressive symptoms, it is also important to address quality of life in patients with mild cognitive impairment.
Disclosure of InterestNone Declared
Intelligence Quotient changes over 10 years: diversity of cognitive profiles in first episode of psychosis and healthy controls
- N. Murillo-Garcia, V. Ortíz-García de la Foz, M. Miguel-Corredera, E. Setién-Suero, K. Neergaard, J. Moya-Higueras, B. Crespo-Facorro, R. Ayesa-Arriola
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S630
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The evidence on the course of the intelligence quotient (IQ) at the long term in individuals with schizophrenia spectrums disorders is inconclusive.
ObjectivesWe aimed to analyse whether IQ improves, declines, or remains stable over 10 years in a sample of patients with First Episode Psychosis (FEP) and healthy controls (HCs).
MethodsThe FEP patients participated in a Program of First Episode Psychosis in Spain called PAFIP. At baseline, FEP patients provided demographic and clinical data, and completed a neuropsychological assessment that included an estimation of premorbid IQ trough the WAIS vocabulary subtest. At 10-year follow-up, the participants were invited to complete the same evaluation and 10-year IQ was estimated. The group of HCs underwent the same neuropsychological battery at both moments. Cluster analysis was performed separately in the FEP patients and the HCs to determine their profiles of intellectual change.
ResultsFEP patients (n=137) were grouped into five clusters (see Figure 1): “Improved low IQ” (9.49% of patients), “Improved average IQ” (14.6%), “Preserved low IQ” (17.52%), “Preserved average IQ” (43.06%), and “Preserved high IQ” (15.33%). Ninety HCs were grouped into three clusters: “Preserved low IQ” (32.22% of the HC), “Preserved average IQ” (44.44%), and “Preserved high IQ” (23.33%). Demographic data of FEP patients are presented in Table 1.
Table 1. Sociodemographic data of FEP patients Improved low IQ Improved average IQ Preserved low IQ Preserved average IQ Preserved high IQ (C1) (C2) (C3) (C4) (C5) N= 13 N= 20 N= 24 N= 59 N= 21 Mean (SD) Mean (SD) Mean (SD) Mean (SD) Mean (SD) F P Premorbid IQ 71.15 (6.50) 84.50 (5.10) 88.96 (5.31) 100.76 (4.90) 117.14 (7.34) 180.87 <0.001 10-year IQ 85.38 (5.94) 103.25 (4.06) 90.00 (5.32) 105.76 (6.49) 114.52 (6.87) 77.47 <0.001 Age 26.44 (6.07) 24.85 (4.08) 25.99 (8.49) 30.86 (9.54) 33.20 (8.81) 4.350 0.002 Age of onset 25.54 (5.81) 24.11 (4.19) 25.46 (8.41) 29.68 (9.26) 32.14 (8.48) 3.993 0.004 Sex (male %) 53.85 80.00 62.50 49.15 42.86 X= 7.672 0.104 Years of education 8.31 (2.14) 9.00 (2.10) 9.00 (2.13) 11.63 (3.39) 14.38 (3.15) 15.818 <0.001 DUP (months) 10.77 (16.50) 8.94 (9.79) 6.42 (9.47) 14.08 (28.46) 12.77 (20.02) 0.628 0.643 Schizophrenia diagnosis (yes%) 53.84 70.00 70.83 59.32 57.14 2.096 0.718 ConclusionsThe FEP patients showed intellectual improvement or stability, but no decline post-onset of psychosis. However, their profiles of intellectual change are more heterogeneous than that of HCs over 10 years. Particularly, there is a subgroup of FEP patients with a significant potential for long-term cognitive enhancement.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
“Keeping an eye on amylase”. Side effects of antidepressants
- T. Jiménez Aparicio, G. Medina Ojeda, A. Rodríguez Campos, L. Rodríguez Andrés, C. Vallecillo Adame, C. De Andrés Lobo, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. J. Mateos Sexmero, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M. P. Pando Fernández, P. Martínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Both in consultations with the general practitioner and with the psychiatrist, antidepressants are one of the most used drugs (1). These have multiple indications, and there are different groups according to their mechanism of action. In relation to this case, we are going to talk about Venlafaxine, a dual-type antidepressant, that is, it inhibits the reuptake of serotonin and norepinephrine. One of the most common side effects is digestive discomfort, which usually resolves after a few weeks (2). However, we should not ignore these symptoms, since they can hide something more serious.
ObjectivesPresentation of a clinical case on a patient who presented an increase in pancreatic amylase after starting treatment with Venlafaxine.
MethodsBibliographic review including the latest articles in Pubmed on side effects of antidepressant treatment, and more specifically at the gastrointestinal level (in this case we will talk about pancreatitis).
ResultsWe present the case of a 49-year-old woman, who was hospitalized 2 years ago, due to a first depressive episode. During this admission, psychopharmacological treatment was started for the first time, on that occasion with a selective serotonin reuptake inhibitor (SSRI), treatment of first choice (3). The patient had no side effects at that time, but the response was very modest, so it was decided to replace that antidepressant with Venlafaxine (with dual action), up to 150mg. The depressive symptoms improved markedly, however the patient began to feel digestive discomfort (which at first did not seem to be of great importance). A general analysis was performed, in which an increase in lipase (978 U/L) and amylase (528 U/L) was detected. An echoendoscopy, an abdominal scan, and a magnetic resonance cholangiography were performed; Pancreatitis secondary to drugs was suspected (a severe condition). Luckily, no significant lesions were found in the tests, and the levels of amylase and lipase decreased when Venlafaxine treatment was withdrawn (without reaching the normal range). The patient was discharged and continued to attend consultations. In the last control, amylase had dropped to 225 U/L. His abdominal pain disappeared. Treatment with Vortioxetine (a multimodal antidepressant) was started, however the amylase levels continue to be monitored, and the patient continues to see the gastroenterologist.
ConclusionsGastrointestinal side effects are very common when taking antidepressant treatment, and in most cases they do not usually represent a serious problem.
However, it is described in the scientific literature that in some cases, acute pancreatitis secondary to some drugs, including Venlafaxine, can occur (4). In order to detect it, it is necessary to perform a blood test and sometimes also other complementary tests.
For its treatment, the fundamental thing is to withdraw the causing drug, trying to find other alternatives, and carry out a control to monitor possible complications
Disclosure of InterestNone Declared
GR.2 A deep intronic FGF14 GAA repeat expansion causes late-onset cerebellar ataxia
- D Pellerin, MC Danzi, C Wilke, M Renaud, S Fazal, M Dicaire, CK Scriba, C Ashton, C Yanick, D Beijer, A Rebelo, C Rocca, Z Jaunmuktane, JA Sonnen, R Larivière, D Genis, L Porcel, K Choquet, R Sakalla, S Provost, M Tétreault, SJ Reiling, S Nagy, V Nishadham, M Purushottam, S Vengalil, M Bardhan, A Nalini, Z Chen, J Mathieu, R Massie, CH Chalk, A Lafontaine, F Evoy, M Rioux, J Ragoussis, KM Boycott, M Dubé, A Duquette, H Houlden, G Ravenscroft, NG Laing, P Lamont, MA Saporta, R Schüle, L Schöls, R La Piana, M Synofzik, S Zuchner, B Brais
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue s2 / June 2023
- Published online by Cambridge University Press:
- 05 June 2023, p. S46
-
- Article
-
- You have access Access
- Export citation
-
Background: The late-onset cerebellar ataxias (LOCAs) have until recently resisted molecular diagnosis. Contributing to this diagnostic gap is that non-coding structural variations, such as repeat expansions, are not fully accessible to standard short-read sequencing analysis. Methods: We combined bioinformatics analysis of whole-genome sequencing and long-read sequencing to search for repeat expansions in patients with LOCA. We enrolled 66 French-Canadian, 228 German, 20 Australian and 31 Indian patients. Pathogenic mechanisms were studied in post-mortem cerebellum and induced pluripotent stem cell (iPSC)-derived motor neurons from 2 patients. Results: We identified 128 patients who carried an autosomal dominant GAA repeat expansion in the first intron of the FGF14 gene. The expansion was present in 61%, 18%, 15% and 10% of patients in the French-Canadian, German, Australian and Indian cohorts, respectively. The pathogenic threshold was determined to be (GAA)≥250, although incomplete penetrance was observed in the (GAA)250-300 range. Patients developed a slowly progressive cerebellar syndrome at an average age of 59 years. Patient-derived post-mortem cerebellum and induced motor neurons both showed reduction in FGF14 RNA and protein expression compared to controls. Conclusions: This intronic, dominantly inherited GAA repeat expansion in FGF14 represents one of the most common genetic causes of LOCA uncovered to date.
Cultural contributions to adults' self-rated mental health problems and strengths: 7 culture clusters, 28 societies, 16 906 adults
- William E. Copeland, Masha Y. Ivanova, Thomas M. Achenbach, Lori V. Turner, Guangyu Tong, Adelina Ahmeti-Pronaj, Alma Au, Monica Bellina, J. Carlos Caldas, Yi-Chuen Chen, Ladislav Csemy, Marina M. da Rocha, Anca Dobrean, Lourdes Ezpeleta, Yasuko Funabiki, Valerie S. Harder, Felipe Lecannelier, Marie Leiner de la Cabada, Patrick Leung, Jianghong Liu, Safia Mahr, Sergey Malykh, Jasminka Markovic, David M. Ndetei, Kyung Ja Oh, Jean-Michel Petot, Geylan Riad, Direnc Sakarya, Virginia C. Samaniego, Sandra Sebre, Mimoza Shahini, Edwiges Silvares, Roma Simulioniene, Elvisa Sokoli, Joel B. Talcott, Natalia Vazquez, Tomasz Wolanczyk, Ewa Zasepa
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 16 / December 2023
- Published online by Cambridge University Press:
- 19 May 2023, pp. 7581-7590
-
- Article
- Export citation
-
Background
It is unknown how much variation in adult mental health problems is associated with differences between societal/cultural groups, over and above differences between individuals.
MethodsTo test these relative contributions, a consortium of indigenous researchers collected Adult Self-Report (ASR) ratings from 16 906 18- to 59-year-olds in 28 societies that represented seven culture clusters identified in the Global Leadership and Organizational Behavioral Effectiveness study (e.g. Confucian, Anglo). The ASR is scored on 17 problem scales, plus a personal strengths scale. Hierarchical linear modeling estimated variance accounted for by individual differences (including measurement error), society, and culture cluster. Multi-level analyses of covariance tested age and gender effects.
ResultsAcross the 17 problem scales, the variance accounted for by individual differences ranged from 80.3% for DSM-oriented anxiety problems to 95.2% for DSM-oriented avoidant personality (mean = 90.7%); by society: 3.2% for DSM-oriented somatic problems to 8.0% for DSM-oriented anxiety problems (mean = 6.3%); and by culture cluster: 0.0% for DSM-oriented avoidant personality to 11.6% for DSM-oriented anxiety problems (mean = 3.0%). For strengths, individual differences accounted for 80.8% of variance, societal differences 10.5%, and cultural differences 8.7%. Age and gender had very small effects.
ConclusionsOverall, adults' self-ratings of mental health problems and strengths were associated much more with individual differences than societal/cultural differences, although this varied across scales. These findings support cross-cultural use of standardized measures to assess mental health problems, but urge caution in assessment of personal strengths.
Cannabis use as a potential mediator between childhood adversity and first-episode psychosis: results from the EU-GEI case–control study
- Giulia Trotta, Victoria Rodriguez, Diego Quattrone, Edoardo Spinazzola, Giada Tripoli, Charlotte Gayer-Anderson, Tom P Freeman, Hannah E Jongsma, Lucia Sideli, Monica Aas, Simona A Stilo, Caterina La Cascia, Laura Ferraro, Daniele La Barbera, Antonio Lasalvia, Sarah Tosato, Ilaria Tarricone, Giuseppe D'Andrea, Andrea Tortelli, Franck Schürhoff, Andrei Szöke, Baptiste Pignon, Jean-Paul Selten, Eva Velthorst, Lieuwe de Haan, Pierre-Michel Llorca, Paulo Rossi Menezes, Cristina M Del Ben, Jose Luis Santos, Manuel Arrojo, Julio Bobes, Julio Sanjuán, Miquel Bernardo, Celso Arango, James B Kirkbride, Peter B Jones, Alexander Richards, Bart P Rutten, Jim Van Os, Isabelle Austin-Zimmerman, Zhikun Li, Craig Morgan, Pak C Sham, Evangelos Vassos, Chloe Wong, Richard Bentall, Helen L Fisher, Robin M Murray, Luis Alameda, Marta Di Forti, EU-GEI WP2 Group
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 04 May 2023, pp. 7375-7384
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Childhood adversity and cannabis use are considered independent risk factors for psychosis, but whether different patterns of cannabis use may be acting as mediator between adversity and psychotic disorders has not yet been explored. The aim of this study is to examine whether cannabis use mediates the relationship between childhood adversity and psychosis.
MethodsData were utilised on 881 first-episode psychosis patients and 1231 controls from the European network of national schizophrenia networks studying Gene–Environment Interactions (EU-GEI) study. Detailed history of cannabis use was collected with the Cannabis Experience Questionnaire. The Childhood Experience of Care and Abuse Questionnaire was used to assess exposure to household discord, sexual, physical or emotional abuse and bullying in two periods: early (0–11 years), and late (12–17 years). A path decomposition method was used to analyse whether the association between childhood adversity and psychosis was mediated by (1) lifetime cannabis use, (2) cannabis potency and (3) frequency of use.
ResultsThe association between household discord and psychosis was partially mediated by lifetime use of cannabis (indirect effect coef. 0.078, s.e. 0.022, 17%), its potency (indirect effect coef. 0.059, s.e. 0.018, 14%) and by frequency (indirect effect coef. 0.117, s.e. 0.038, 29%). Similar findings were obtained when analyses were restricted to early exposure to household discord.
ConclusionsHarmful patterns of cannabis use mediated the association between specific childhood adversities, like household discord, with later psychosis. Children exposed to particularly challenging environments in their household could benefit from psychosocial interventions aimed at preventing cannabis misuse.
The association between reasons for first using cannabis, later pattern of use, and risk of first-episode psychosis: the EU-GEI case–control study
- Edoardo Spinazzola, Diego Quattrone, Victoria Rodriguez, Giulia Trotta, Luis Alameda, Giada Tripoli, Charlotte Gayer-Anderson, Tom P Freeman, Emma C Johnson, Hannah E Jongsma, Simona Stilo, Caterina La Cascia, Laura Ferraro, Daniele La Barbera, Antonio Lasalvia, Sarah Tosato, Ilaria Tarricone, Giuseppe D'Andrea, Michela Galatolo, Andrea Tortelli, Ilaria Tagliabue, Marco Turco, Maurizio Pompili, Jean-Paul Selten, Lieuwe de Haan, Paulo Rossi Menezes, Cristina M Del Ben, Jose Luis Santos, Manuel Arrojo, Julio Bobes, Julio Sanjuán, Miguel Bernardo, Celso Arango, James B Kirkbride, Peter B Jones, Michael O'Donovan, Bart P Rutten, Jim Van Os, Craig Morgan, Pak C Sham, Isabelle Austin-Zimmerman, Zhikun Li, Evangelos Vassos, EU-GEI WP2 Group, Robin M Murray, Marta Di Forti
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 02 May 2023, pp. 7418-7427
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
While cannabis use is a well-established risk factor for psychosis, little is known about any association between reasons for first using cannabis (RFUC) and later patterns of use and risk of psychosis.
MethodsWe used data from 11 sites of the multicentre European Gene-Environment Interaction (EU-GEI) case–control study. 558 first-episode psychosis patients (FEPp) and 567 population controls who had used cannabis and reported their RFUC.
We ran logistic regressions to examine whether RFUC were associated with first-episode psychosis (FEP) case–control status. Path analysis then examined the relationship between RFUC, subsequent patterns of cannabis use, and case–control status.
ResultsControls (86.1%) and FEPp (75.63%) were most likely to report ‘because of friends’ as their most common RFUC. However, 20.1% of FEPp compared to 5.8% of controls reported: ‘to feel better’ as their RFUC (χ2 = 50.97; p < 0.001). RFUC ‘to feel better’ was associated with being a FEPp (OR 1.74; 95% CI 1.03–2.95) while RFUC ‘with friends’ was associated with being a control (OR 0.56; 95% CI 0.37–0.83). The path model indicated an association between RFUC ‘to feel better’ with heavy cannabis use and with FEPp-control status.
ConclusionsBoth FEPp and controls usually started using cannabis with their friends, but more patients than controls had begun to use ‘to feel better’. People who reported their reason for first using cannabis to ‘feel better’ were more likely to progress to heavy use and develop a psychotic disorder than those reporting ‘because of friends’.






